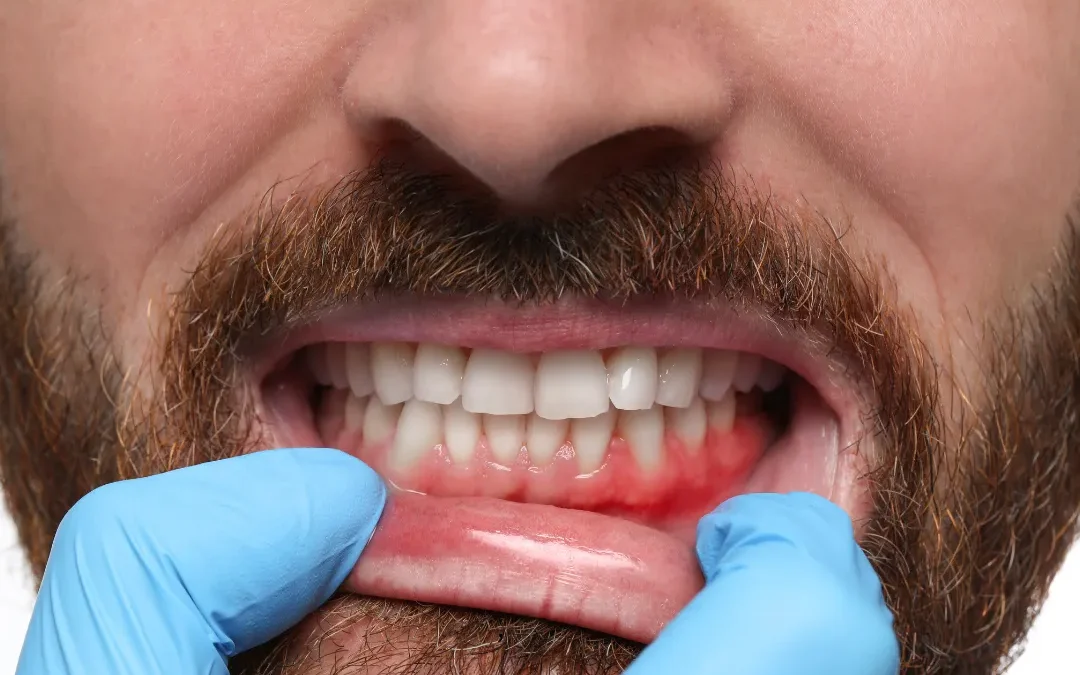
Oral health is a crucial part of your overall well-being, yet many people overlook the importance of healthy gums. Gum disease and gingivitis are common but serious conditions that can lead to tooth loss, bone damage, and even impact your general health. If left untreated, they can progress and result in complications far beyond your mouth. Did you know that 47% of adults over 30 have some form of gum disease? This blog post will help you understand gum disease and gingivitis, how they differ, their causes, symptoms, treatments, and prevention methods.
What Is Gum Disease (Periodontitis)?
Gum disease, also known as periodontitis, is a severe gum infection that damages the soft tissue and destroys the bone that supports your teeth. Unlike gingivitis, which is reversible, gum disease is progressive and, without proper treatment, can lead to permanent tooth loss. Periodontitis develops when gingivitis goes untreated, and bacteria infiltrate the deeper layers of the gum, leading to inflammation and infection.
Effects on Gums and Bone
In its early stages, gum disease can cause swollen and tender gums. As it progresses, the infection spreads deeper, leading to the formation of gum pockets. These pockets trap food particles and plaque, which further exacerbate the disease. Over time, the infection can erode the bone that supports your teeth, leading to tooth mobility and eventual tooth loss.
Complications
If left untreated, periodontitis can cause further complications beyond your gums and teeth. The infection can enter your bloodstream, increasing your risk of developing heart disease, stroke, and even worsening diabetes. It’s crucial to catch gum disease early before it leads to more severe health issues.
What Is Gingivitis?
Gingivitis is the earliest stage of gum disease and typically causes inflammation of the gums due to bacterial plaque buildup. It’s the most common form of gum disease and is usually harmless if treated promptly. Gingivitis affects only the gums and does not lead to the destruction of bone or tissue that supports the teeth. However, if left untreated, it can progress into periodontitis, which causes irreversible damage.
Gingivitis is often caused by poor oral hygiene that encourages plaque to form on teeth, leading to inflammation. Plaque is a sticky film of bacteria that builds up on your teeth, and if it’s not removed by brushing and flossing, it can lead to gum infection.
Do You Have Gingivitis? Take Our Quiz
- Red, swollen gums that may bleed when brushing or flossing.
- Bad breath or a bad taste in your mouth.
- Tender gums that feel sore to the touch.
- Gums that appear to recede from the teeth, leaving them more exposed.
If you answered yes to any of the above, you may have gingivitis. Don’t worry! Gingivitis is treatable, and we can help. Book an appointment with our experts at Parramatta Green Dental for a professional evaluation and cleaning.
How Gingivitis Progresses to Periodontitis
While gingivitis is reversible, periodontitis is an irreversible condition. If gingivitis is left untreated for too long, the infection spreads deeper into the gums, affecting the supporting structures of your teeth. This progression is what transforms gingivitis into periodontitis.
The Role of Plaque and Tartar
Plaque is the primary cause of gingivitis, but when it’s not removed, it hardens into tartar (also known as calculus). Tartar cannot be removed by brushing alone and requires professional cleaning. Tartar buildup around the gums provides an ideal environment for bacteria to thrive, causing infection to spread to the deeper layers of your gums. As the disease progresses, it can lead to tooth mobility and, in severe cases, tooth loss.
Gum Pockets
As periodontitis develops, gum pockets form between your teeth and gums. These pockets become filled with plaque, tartar, and bacteria, further aggravating the infection. The deeper the pockets, the more difficult it becomes to clean them, leading to a vicious cycle of infection and further damage to the gums and bone structure.
Key Differences Between Gingivitis and Periodontitis
Although both gingivitis and periodontitis are forms of gum disease, they differ significantly in severity and consequences.
Gingivitis: Reversible and Focused on the Gums
- Location: Gingivitis only affects the gums and is limited to the surface level of the gums.
- Symptoms: Swollen, red, and bleeding gums that cause discomfort but no permanent damage.
- Reversibility: Gingivitis can be fully reversed with proper dental care, including brushing, flossing, and regular professional cleanings.
Periodontitis: Irreversible and Affects Bone and Gums
- Location: Periodontitis affects the gums, bone, and ligaments that support the teeth.
- Symptoms: Severe gum recession, tooth mobility, bad breath, and the formation of gum pockets.
- Irreversibility: Periodontitis cannot be completely reversed. However, with treatment, it can be managed to prevent further damage.
Symptoms of Gum Disease
Understanding the symptoms of gum disease is crucial to recognising the problem early. The earlier you spot these signs, the sooner you can seek treatment to prevent further damage. Both gingivitis and periodontitis have distinct symptoms, though some overlap.
Common Signs of Gingivitis
Gingivitis is the mildest form of gum disease, but it’s important to be aware of its symptoms for early intervention. Key signs of gingivitis include:
- Red, swollen gums: Gums may appear puffy or inflamed.
- Bleeding gums: You may notice blood when brushing or flossing.
- Bad breath: Persistent bad breath (halitosis) that doesn’t go away even after brushing.
- Tender gums: Gums that feel sore or sensitive to the touch.
Though gingivitis is typically not painful, bleeding or swollen gums should not be ignored. If caught early, it can be completely reversed with professional cleaning and improved oral hygiene.
Symptoms of Periodontitis
Periodontitis is a more severe form of gum disease and can lead to significant damage if left untreated. It often causes the following symptoms:
- Receding gums: Gums may start to pull away from your teeth, making the teeth appear longer.
- Gum pockets: Deep pockets between the gums and teeth form, which can trap food particles and plaque.
- Loose teeth: As the infection progresses, teeth may become loose due to bone loss.
- Bad breath (halitosis): A persistent, foul-smelling breath that doesn’t improve with brushing.
- Pain while chewing: Pain or discomfort while chewing can be an indication of advanced gum disease.
If you experience any of these symptoms, it’s essential to visit a dentist as soon as possible. Periodontitis is irreversible, but with proper care, the progression of the disease can be slowed, and further damage can be minimised.
Risk Factors for Developing Gum Disease
While gum disease is common, several risk factors can increase your likelihood of developing it. Some of these factors are controllable, while others are not. Understanding these risk factors can help you make informed decisions to protect your gum health.

Poor Oral Hygiene: The Leading Cause of Gum Disease
The primary cause of gum disease is plaque buildup, which forms on your teeth and gums from the food and drinks you consume. Without regular brushing and flossing, plaque can harden into tartar, which can only be removed by a dentist. This leads to gum infection and disease.
Smoking and Tobacco Use
Smoking is one of the most significant risk factors for gum disease. Tobacco products reduce blood flow to the gums, making it harder for your gums to heal and fight infection. Smokers are more likely to develop gum disease and experience more severe symptoms compared to non-smokers.
Diabetes: A Compounding Factor
People with diabetes are more susceptible to gum disease due to the impact of high blood sugar on the body’s immune response. Poorly controlled diabetes weakens the body’s ability to fight infection, increasing the likelihood of gum disease and delaying healing.
Hormonal Changes: Pregnancy, Puberty, and Menopause
Changes in hormones can affect gum health. During pregnancy, puberty, and menopause, hormonal fluctuations can make gums more sensitive, increasing the risk of gingivitis and periodontitis. Pregnant women, in particular, may experience “pregnancy gingivitis,” which can lead to swollen and bleeding gums.
Medications and Health Conditions
Certain medications, such as those used for high blood pressure or depression, can cause dry mouth, reducing the amount of saliva that helps cleanse the mouth and control bacteria. Medications that affect the immune system can also increase the risk of gum disease.
Stress, Poor Nutrition, and Other Factors
Chronic stress can weaken the immune system, making it harder for your body to fight off gum infections. Additionally, a poor diet lacking in vitamins like Vitamin C can impair gum health and make them more susceptible to infection. 5 best Vitamins are essential for managing the disease and preventing it from returning.
Diagnosis and Dental Assessment for Gum Disease
If you notice any symptoms of gum disease, it’s important to visit a dentist for an evaluation. Early diagnosis can prevent the condition from worsening and help you take the necessary steps toward treatment.
How Dentists Diagnose Gum Disease
When you visit the dentist, they will conduct a comprehensive exam to check for signs of gum disease. This may include:
- Checking for gum bleeding: A dentist will gently probe your gums to check for bleeding, which is an early sign of gingivitis.
- Measuring pocket depth: A small instrument called a periodontal probe is used to measure the depth of the pockets around your teeth. Deeper pockets indicate more severe gum disease.
- X-rays: X-rays help assess the extent of bone loss, a common complication of advanced periodontitis.
Tools Used in Diagnosis
- Periodontal probe: Used to measure gum pocket depth and assess the health of the gums.
- X-rays: Help to detect bone loss and hidden infection beneath the gum line.
- Visual examination: The dentist looks for obvious signs of gum inflammation, swelling, or recession.
Treatments for Gingivitis and Periodontitis
Both gingivitis and periodontitis require professional dental treatment to manage the condition and prevent further damage. The treatments for each condition differ based on the severity of the disease.
Treatment for Gingivitis
Gingivitis is reversible, and treatment typically involves:
- Professional cleaning: A dentist or hygienist will remove plaque and tartar buildup through a procedure called scaling and root planing. This deep cleaning helps prevent the infection from spreading.
- Improved home care: Brushing twice a day, flossing daily, and using antimicrobial mouthwash can help prevent the recurrence of gingivitis.
Treatment for Periodontitis
Can gum disease be reversed? While periodontitis cannot be fully reversed, it can be managed with advanced treatments, including:
- Scaling and root planing: Deep cleaning to remove plaque and tartar from below the gumline and smooth the tooth roots to prevent further buildup.
- Antibiotics: Topical or oral antibiotics may be prescribed to help control infection and inflammation.
- Surgical treatments: In severe cases, flap surgery or bone grafting may be required to restore the gums and bone.
- Laser treatments: Lasers can help remove infected tissue and promote faster healing.
Ongoing Care and Maintenance
After treatment, regular dental cleanings and check-ups are essential for maintaining gum health. Your dentist will monitor your gums closely to ensure the disease doesn’t return and that your gums remain healthy.
Simple Steps to Prevent Gum Disease
Prevention is the best strategy to avoid gum disease. By adopting good oral hygiene habits, making healthier lifestyle choices, and scheduling regular dental check-ups, you can significantly reduce your risk of developing gingivitis or periodontitis.
Brushing and Flossing: Key to Healthy Gums
You can make a big difference in your gum health by brushing and flossing daily. Brush your teeth twice a day with fluoridated toothpaste and use interdental brushes or floss to clean between your teeth. These simple habits can prevent plaque buildup and help you maintain healthy gums.
Dental Hygiene Tools
- Soft toothbrush: Use a soft-bristle toothbrush to avoid damaging your gums.
- Interdental brushes and floss: These tools help clean the areas between your teeth that your toothbrush can’t reach.
- Antimicrobial mouthwash: Helps kill bacteria and prevent plaque buildup.
Regular Dental Check-ups
Regular visits to your dentist for professional cleaning and evaluation are crucial for detecting gum disease early. Your dentist can remove tartar, which you can’t do at home, and ensure your gums stay healthy.
Lifestyle Adjustments
- Quit smoking: Smoking is a major risk factor for gum disease. Quitting helps your gums heal and reduces your risk of complications.
- Eat a balanced diet: Include plenty of Vitamin C, Calcium, and Vitamin D in your diet to support strong, healthy gums.
Prognosis for Gum Disease
Understanding the prognosis for gum disease and gingivitis is essential for managing your oral health. The outlook can vary significantly depending on how early the condition is diagnosed, how diligently you follow treatment plans, and how committed you are to maintaining good oral hygiene.
Early Detection and Treatment for Gingivitis
If gingivitis is detected early and treated promptly, the prognosis is excellent. With professional cleaning and better home care, you can expect the inflammation to subside, and your gums will return to a healthy state. The key is to address it before it progresses to periodontitis, which would result in more complex treatment and long-term care.
Managing Periodontitis
Although periodontitis is irreversible, it can still be managed effectively with ongoing treatment. The goal is to stop the disease from progressing further, preventing tooth loss and additional bone damage. Regular maintenance cleanings, along with a dedicated at-home oral hygiene routine, are critical for keeping the condition under control. If you have advanced periodontitis, surgery or other procedures may be necessary, but with proper care, you can maintain your teeth for many years.
Maintaining Healthy Gums for Life
Whether you’re managing gingivitis or periodontitis, the most important part of the treatment is consistent care. Continued professional monitoring and at-home maintenance, including regular dental visits, brushing, flossing, and possibly even specialised treatments like deep cleanings, can ensure you maintain healthy gums for life. Remember, the key to success is prevention, early detection, and ongoing care. If gum disease has affected the appearance of your smile, Porcelain Veneers can restore your smile’s aesthetic appeal.
Frequently Asked Questions About Gum Disease
1. What Is the Difference Between Gingivitis and Periodontitis?
- Gingivitis is the early, reversible stage of gum disease, affecting only the gums and causing inflammation and bleeding. If treated early, it can be reversed with good oral hygiene and professional cleaning.
- Periodontitis is the advanced, irreversible stage of gum disease, which affects both the gums and bone, causing severe damage, gum recession, and tooth loss if left untreated.
2. Can Gum Disease Be Reversed?
Gingivitis can be fully reversed with the right treatment and care. Periodontitis cannot be completely reversed, but it can be managed and controlled with treatments such as scaling and root planing, antibiotics, and sometimes surgery.
3. Is Gum Disease Painful?
Gingivitis is typically not painful, although bleeding and swollen gums can be uncomfortable. Periodontitis, on the other hand, can be painful, especially when there is gum recession or infection deep in the tissues.
4. How Can I Prevent Gum Disease?
- Good oral hygiene is the most important factor in preventing gum disease. Brush your teeth twice a day, floss daily, and use antimicrobial mouthwash.
- Regular dental check-ups are essential to remove tartar buildup and detect any early signs of gum disease.
- A healthy diet and quitting smoking also significantly reduce the risk of developing gum disease.
5. How Often Should I See a Dentist for Gum Disease Prevention?
Regular dental check-ups should occur at least every six months. However, if you have a history of gum disease or are at a higher risk (e.g., due to smoking, diabetes, or hormonal changes), your dentist may recommend more frequent visits.
How Parramatta Green Dental Can Help
At Parramatta Green Dental, we understand the importance of maintaining healthy gums, and we are committed to providing expert care to help you achieve and maintain optimal oral health. Whether you’re dealing with early signs of gingivitis or advanced periodontitis, our skilled team is here to support you every step of the way. Here’s how we can help:
Comprehensive Gum Disease Treatment
Our practice offers a full range of services to treat both gingivitis and periodontitis. We provide:
- Professional cleanings (scaling and root planing) to remove plaque and tartar buildup.
- Advanced treatments like laser therapy, surgical procedures, and bone grafts for more severe cases of periodontitis.
- Personalised care plans tailored to your specific needs, ensuring the best results for your gum health.
Preventive Care and Maintenance
Prevention is always better than treatment, which is why we focus on educating our patients about the importance of regular dental check-ups and good oral hygiene. We provide:
- Comprehensive exams to check for signs of gum disease.
- Ongoing support with maintenance cleanings to keep your gums healthy and catch any early signs of disease before they progress.
Patient Education and Support
Our team at Parramatta Green Dental is always available to answer your questions and guide you through the process of managing and preventing gum disease. We believe in providing clear, easy-to-understand advice so that you feel confident in caring for your oral health.
If you’re experiencing any symptoms of gum disease or want to ensure you’re on the right path to maintaining healthy gums, don’t hesitate to schedule an appointment with us. We are conveniently located in Parramatta, and we’re here to help you keep your smile bright and healthy!
Conclusion: Prioritise Your Gum Health
Your gums play an essential role in your overall oral health. By understanding the difference between gingivitis and periodontitis, recognising the symptoms early, and seeking the right treatment, you can protect your gums from long-term damage. Regular check-ups and good oral hygiene are the best ways to prevent gum disease and maintain your healthy smile.
If you have any concerns about your gum health or need professional treatment, Parramatta Green Dental is here to help. Schedule an appointment with us today and take the first step towards a healthier, happier smile. Early diagnosis of gum disease can save you from painful and expensive treatments later